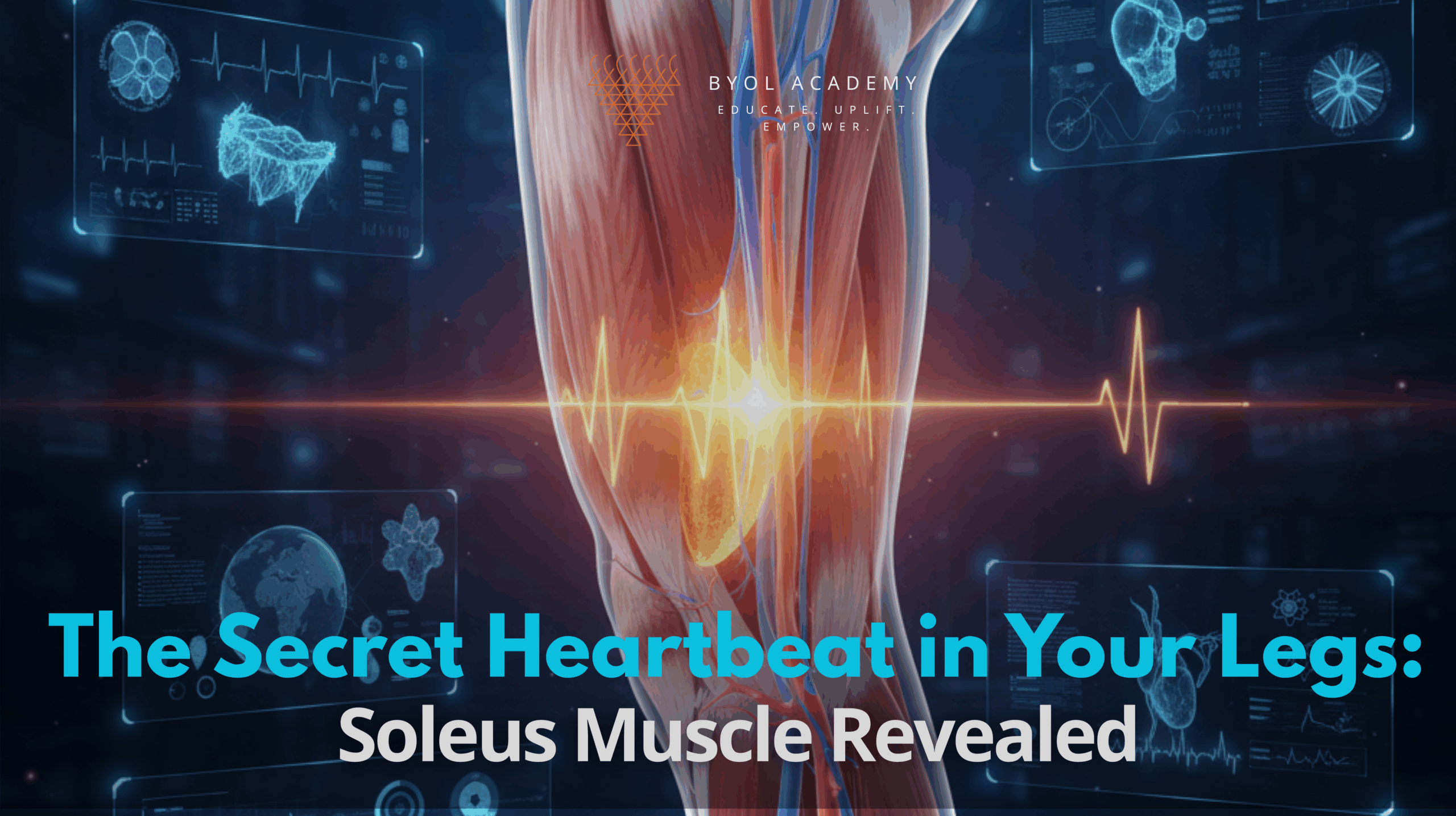
The calf muscle, often overlooked in daily life, plays a critical role in maintaining healthy circulation and overall cardiovascular function. […]
Fetal Cells in Maternal Heart Repair: A Natural Mechanism for Cardiac Regeneration
Pregnancy is a remarkable biological phenomenon, not only because it sustains the development of a new life, but also because it initiates complex cellular interactions between the mother and the fetus. One of the most intriguing of these is fetal-maternal microchimerism, the presence of fetal cells in maternal tissues long after delivery has emerged as a fascinating mechanism with potential implications for tissue repair.
Recent research, particularly the study “Fetal Cells Traffic to Injured Maternal Myocardium and Undergo Cardiac Differentiation”, demonstrates that fetal cells can actively home to injured maternal hearts, differentiate into multiple cardiac lineages, and contribute to functional tissue repair, offering a unique perspective on regenerative medicine.
Understanding Fetal-Maternal Microchimerism
Microchimerism occurs when two genetically distinct populations of cells coexist within the same tissue or organism. In pregnancy, fetal cells cross into the mother’s bloodstream, with some demonstrating multilineage potential and the ability to differentiate into various cell types. Fetal-derived cells identified in maternal blood and tissues include hematopoietic stem/progenitor cells (CD34+, CD38+), mononuclear cells (CD3+, CD14+), lymphoid progenitors (CD19+, IgM+), and mesenchymal stem cells (desmin+), among others. Evidence from animal studies has demonstrated that these cells can migrate to sites of injury in organs such as the brain, liver, kidney, and lung, participating in tissue regeneration and neoangiogenesis.
Despite this understanding, the potential role of fetal cells in maternal cardiac repair had remained unexplored until now.
Clinical Observations Driving the Hypothesis
Peripartum cardiomyopathy, a rare but severe form of heart failure occurring in late pregnancy or postpartum, presents an unusual paradox: despite significant myocardial injury, many patients recover cardiac function, sometimes completely. This observation led researchers to hypothesize that fetal cells in maternal circulation may home to injured hearts and contribute to regeneration, potentially explaining these remarkable recoveries.
Experimental Design and Methodology
To explore this hypothesis, researchers conducted a series of in vivo and in vitro experiments:
1. Animal Model: Pregnant mice carrying eGFP-tagged fetuses were used, allowing fetal cells to be tracked within maternal tissues.
2. Induction of Cardiac Injury: Maternal mice were subjected to experimental myocardial infarction, creating a controlled model of heart damage.
3. Tracking Fetal Cells: The presence and distribution of fetal cells in maternal hearts were assessed using fluorescence imaging and molecular assays.
4. Differentiation and Function: Fetal cells were isolated from maternal hearts and analyzed for differentiation into cardiomyocytes, endothelial cells, and smooth muscle cells. Functional integration was evaluated in vitro through vascular tube formation and spontaneous beating cardiomyocyte assays.
5. Stemness and Lineage Markers: Expression of cardiac, endothelial, and pluripotency markers, including Cdx2, Nkx2.5, CD31, Sca-1, c-Kit, Islet1, Nanog, Sox2 was assessed to determine lineage commitment and stem cell potential.
Key Findings
1. Targeted Homing to Injured Myocardium
Fetal cells did not distribute randomly; they selectively migrated to areas of myocardial injury, confirming that maternal tissue injury provides signals that attract fetal progenitor cells.
2. Multilineage Differentiation
Cardiomyocytes: Fetal cells differentiated into functional heart muscle cells, evidenced by expression of cardiac troponin T and formation of gap junctions (connexin-43).
Endothelial Cells: Cells formed vascular structures both in vivo and in 3D collagen matrices in vitro.
Smooth Muscle Cells: Contributed to vascular architecture, supporting neoangiogenesis.
3. Functional Maturation
- Isolated fetal cells formed vascular tubes in vitro, demonstrating angiogenic potential.
- When co-cultured with neonatal cardiomyocytes, some fetal cells spontaneously contracted, confirming functional cardiomyocyte differentiation.
- Importantly, this differentiation occurred without cell fusion, indicating true lineage commitment rather than hybridization with maternal cells.
4. Identification of Novel Stem Cell Populations
Approximately 40% of fetal cells expressed Cdx2, a marker traditionally associated with trophoblast stem cells, previously thought to only contribute to the placenta.
Other markers confirmed the presence of multipotent and pluripotent cell populations, capable of differentiating into multiple cardiac lineages.
Implications for Regenerative Medicine
These findings suggest a naturally occurring regenerative system mediated by fetal cells:
- Therapeutic Potential: Cdx2+ fetal cells may represent a novel source of stem cells for cardiovascular therapies, potentially enabling new strategies for myocardial infarction and heart failure treatment.
- Maternal-Fetal Biology: The study demonstrates a mutualistic interaction, where fetal cells actively contribute to maternal tissue repair, expanding our understanding of pregnancy biology.
- Stem Cell Research: This work supports the concept that non-embryonic stem cells can differentiate into beating cardiomyocytes, challenging previous paradigms in regenerative biology.
Challenges and Future Directions
While promising, several issues need careful consideration:
- Translation to Humans: Human studies are required to confirm whether fetal cells behave similarly in maternal hearts.
- Mechanistic Insights: The molecular signals guiding fetal cell homing and differentiation remain to be elucidated.
- Safety and Integration: Long-term safety, immune compatibility, and functional integration in vivo must be rigorously evaluated.
- Clinical Applications: Controlled isolation and expansion of Cdx2+ fetal cells for therapeutic use are required before clinical translation.
Conclusion
The study “Fetal Cells Traffic to Injured Maternal Myocardium and Undergo Cardiac Differentiation” reveals a remarkable, naturally occurring regenerative mechanism: fetal cells can migrate to injured maternal hearts, differentiate into multiple cardiac lineages, and functionally contribute to tissue repair.
The identification of Cdx2+ trophoblast-like stem cells opens exciting opportunities for novel cell-based therapies targeting cardiovascular diseases and provides a deeper understanding of maternal-fetal biology. Pregnancy, therefore, may not only be a journey of creating life but also a journey of healing life.
References
- Kara, R. J., Bolli, P., Karakikes, I., Matsunaga, I., Tripodi, J., Tanweer, O., Altman, P., Shachter, N. S., Nakano, A., Najfeld, V., & Chaudhry, H. W. (2012). Fetal Cells Traffic to Injured Maternal Myocardium and Undergo Cardiac Differentiation. Circulation Research, 110(1), 82–93. https://doi.org/10.1161/CIRCRESAHA.111.249037
- Pritchard, S., & Bianchi, D. W. (2012). Fetal cell microchimerism in the maternal heart: baby gives back. Circulation Research, 110(1), 3–5. https://doi.org/10.1161/CIRCRESAHA.111.260299
- Khosrotehrani, K., Johnson, K. L., Cha, D. H., Salomon, R. N., & Bianchi, D. W. (2004). Transfer of fetal cells with multilineage potential to maternal tissue. JAMA, 292(1), 75–80. https://doi.org/10.1001/jama.292.1.75
- Bianchi, D. W., Zickwolf, G. K., Weil, G. J., Sylvester, S., & DeMaria, M. A. (1996). Male fetal progenitor cells persist in maternal blood for as long as 27 years postpartum. Proceedings of the National Academy of Sciences, 93(2), 705–708. https://doi.org/10.1073/pnas.93.2.705